The following “Change Page” was published in the British Medical Journal on the 3rd November 2014. The authors were: Anne Corbett, Professor Alistair Burns and Professor Clive Ballard.
This is what the British Medical Journal would like be achieved from the “Change Page”:
The following box gives the “bottom line” for this change page:
The bottom line:
-
Despite continued use of antipsychotics to treat agitation and aggression in people with dementia there is limited evidence of clinically meaningful benefit
-
The potential harms of antipsychotic use (including increased cerebrovascular events and mortality) outweigh the benefits
-
Risperidone is the only recommended antipsychotic, and should be used only in people with dementia who have pre-existing psychotic disorders or severe aggression. It should be prescribed for no more than 12 weeks
-
Careful monitoring is the best practice alternative, with evidence that alternative treatments including analgesia and non-drug based approaches provide effective options
In response to this “Change Page” I submitted the following to the British Medical Journal:
And here is my response in html form with a few images added:
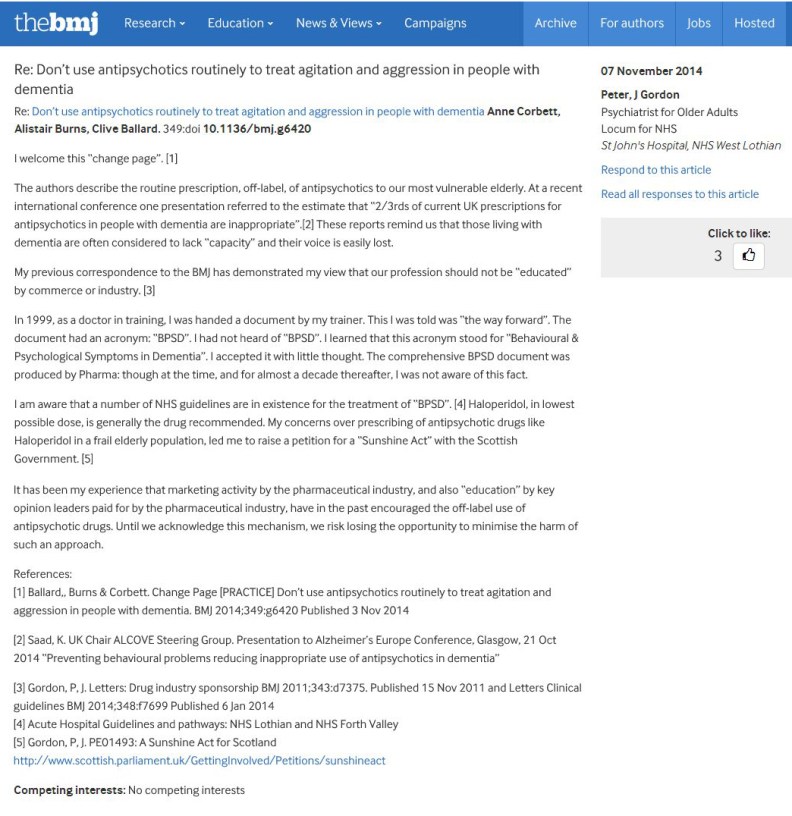
I welcome this “change page”.[1]
The authors describe the routine prescription, off-label, of antipsychotics to our most vulnerable elderly. At a recent international conference one presentation referred to the estimate that “2/3rds of current UK prescriptions for antipsychotics in people with dementia are inappropriate”.[2] These reports remind us that those living with dementia are often considered to lack “capacity” and their voice is easily lost.
My previous correspondence to the BMJ has demonstrated my view that our profession should not be “educated” by commerce or industry.[3]
In 1999, as a doctor in training, I was handed a document by my trainer. This I was told was “the way forward”. The document had an acronym: “BPSD”. I had not heard of “BPSD”. I learned that this acronym stood for “Behavioural & Psychological Symptoms in Dementia”. I accepted it with little thought. The comprehensive BPSD document was produced by Pharma: though at the time, and for almost a decade thereafter, I was not aware of this fact.
I am aware that a number of NHS guidelines are in existence for the treatment of “BPSD”.[4] Haloperidol, in lowest possible dose, is generally the drug recommended. My concerns over prescribing of antipsychotic drugs like Haloperidol in a frail elderly population, led me to raise a petition for a “Sunshine Act” with the Scottish Government.[5]
It has been my experience that marketing activity by the pharmaceutical industry, and also “education” by key opinion leaders paid for by the pharmaceutical industry, have in the past encouraged the off-label use of antipsychotic drugs. Until we acknowledge this mechanism, we risk losing the opportunity to minimise the harm of such an approach.
[1] Ballard,, Burns & Corbett. Change Page [PRACTICE] Don’t use antipsychotics routinely to treat agitation and aggression in people with dementia. BMJ 2014;349:g6420 Published 3 Nov 2014
[2] Saad, K. UK Chair ALCOVE Steering Group. Presentation to Alzheimer’s Europe Conference, Glasgow, 21 Oct 2014 “Preventing behavioural problems reducing inappropriate use of antipsychotics in dementia”
[3] Gordon, P, J. Letters: Drug industry sponsorship BMJ 2011;343:d7375. Published 15 Nov 2011 and Letters Clinical guidelines BMJ 2014;348:f7699 Published 6 Jan 2014
[4] Acute Hospital Guidelines and pathways: NHS Lothian and NHS Forth Valley
[5] Gordon, P, J. PE01493: A Sunshine Act for Scotland
From NHS England bio: “Professor Alistair Burns is Professor of Old Age Psychiatry and Vice Dean for the Faculty of Medical and Human Sciences at The University of Manchester. He is an Honorary Consultant Old Age Psychiatrist in the Manchester Mental Health and Social Care Trust (MMHSCT) and is the National Clinical Director for Dementia and Older Peoples’ Mental Health, NHS England.”
It is clear that Professor Alistair Burns has been thoroughly scrupulous in making declarations which confirm that he personally has had no financial competing interests since he took up post as National Clinical Director for Dementia (NHS England).
Prior to this, Professor Burns worked most extensively with the pharmaceutical industry and his declarations can be found with each of the research papers in which he was involved:
Here are other Psychiatrists and Academic involved in Psychiatry for Older Adults [the following is based on declarations that they have given in published research papers]: